News
Parasites Can Suppress Onset of Type 1 Diabetes with "Sugar"
Hopes for New Preventive and Therapeutic Methods
Updated in June 2021
Type 1 diabetes is a chronic disease in which insulin─a type of hormone─cannot be produced due to abnormal immune function. This can result in hyperglycemia or high blood sugar. People of all ages, especially children and adolescents, are suffering from the disease. Against this backdrop, research groups from RIKEN and other institutes have achieved remarkable results. They have identified immune cells that suppress the onset of the disease, and found that “sugar" secreted by helminth parasites living inside the intestines holds the key. This was verified by experiments using mice. Further research raises hope for the development of new preventive and therapeutic treatment for type 1 diabetes.
There are Approximately 100,000 to 140,000 Patients in Japan
Type 1 diabetes is a type of "autoimmune disease" in which the immune system that should protect the body from foreign substances mistakenly attacks one's own cells and tissues. The "beta cells" of the pancreas, which secrete insulin, are destroyed by one’s own immune cells. For this reason, glucose in the blood obtained from food is not taken in by cells and is not converted into energy. This concentration (blood sugar level) rises and is released in urine.
Symptoms include thirst, polyuria, weight loss, and impaired consciousness, which can be life-threatening. Diabetes is difficult to cure completely, and patients need to keep taking insulin injections to control their blood sugar levels. How can we reduce the destruction of the beta cells that cause type 1 diabetes? This is a major research topic.
According to the data compiled by the research group of Japan’s Ministry of Health, Labor and Welfare in 2018, the number of type 1 diabetic patients is estimated to be about 100,000 to 140,000 nationwide. A US study found that the prevalence of type 1 diabetes in people in the US under the age of 20 increased by about 21 percent during the eight years between 2001-09. Type 2 diabetes, which is a lifestyle-related disease common among middle-aged and elderly people, has a completely different mechanism compared to type 1. Even if insulin is released, it does not work sufficiently due to obesity and causes hyperglycemia or a rise in blood sugar.
Teamwork between Parasites and Bacteria
When a drug that destroys beta cells was administered to mice, insulin was not produced and type 1 diabetes occurred. On the other hand, in mice infected with a type of intestinal parasite, beta cells were not destroyed and they did not develop diabetes even if the drug was given.
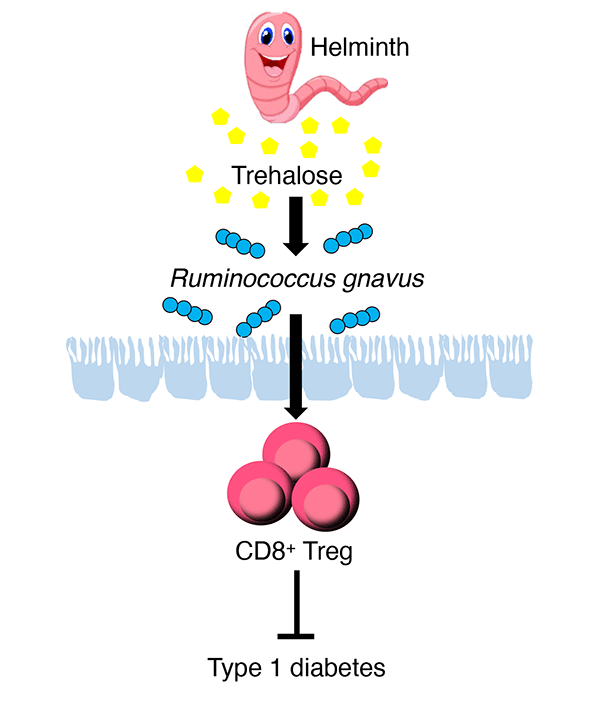
In mice infected with this parasite, a type of immune-suppressing cell, "CD8-positive regulatory T cells” (CD8+ Treg cells), was found to be multiplying. When the CD8+ Treg cells were removed, type 1 diabetes developed. What’s more, the onset was suppressed by inserting CD8+ Treg cells into mice not infected with parasites.
When examining the small intestines of mice infected with these parasites, the team found the parasites secreted the sugar "trehalose", and a type of intestinal bacteria increased by feeding on this sugar. When normal wild mice were fed this bacterial companion, CD8+ Treg cells increased, and administering beta cell-destroying drugs did not lead to type 1 diabetes.
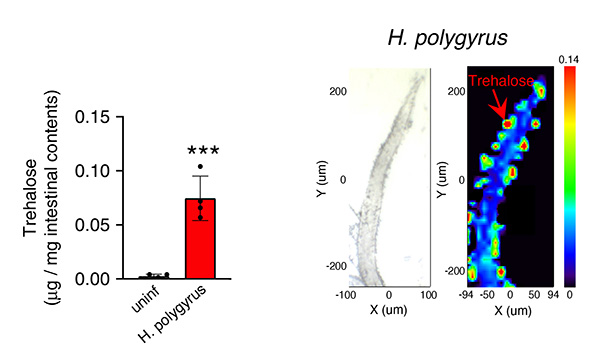
Right: As indicated by the red arrow, the warmer the color, the higher the concentration of trehalose. (provided by RIKEN)
These results indicate that the bacteria feeding on the trehalose secreted by the helminth parasites increases CD8+ Treg cells, stops the destruction of beta cells, and suppresses the onset of the disease. It is almost like the parasites and bacteria are working as a team. Moreover, researchers also found that human patients with type 1 diabetes have low levels of both CD8+ Treg cells and the bacteria used in the mouse experiments.
Oral Medication May Free Patients from Insulin Shots
In another research group's experiment, CD8+ Treg cells were found to be effective against other autoimmune diseases, but the mechanism of their multiplication was unclear. Parasites tend to have a harmful image, but it is surprising to know that some of them can actually protect the human body.
In the future, the group will continue to research the detailed mechanism and function of how CD8+ Treg cells increase and what substances the bacteria produce. As a future clinical application, RIKEN's team leader Ohno Hiroshi (intestinal immunology) said, "We can identify the substances produced by the bacteria and the substances that make up the bacteria to make them into an oral medication. By taking these drugs regularly, type 1 diabetes patients would no longer have to inject insulin."
Verifying the "Hygiene Hypothesis" Theory
While infectious diseases caused by parasites and bacteria have decreased due to better sanitation, modern diseases like allergies and autoimmune diseases such as type 1 diabetes are on the rise. It is also known that the number of patients with autoimmune diseases has actually increased in areas where parasite infections have dramatically decreased due to the spread of drugs. Rises in modern diseases caused by decreases in infectious diseases is called the "hygiene hypothesis." Through this achievement, the research group claims to have proven this hypothesis for the first time, including its mechanism.
The research group consists of RIKEN Center for Biomedical Sciences, Gunma University Graduate School of Medicine, Tokyo Institute of Technology, and National Institute of Infectious Diseases Department of Parasitology. The results were published in the British scientific journal Nature Communications dated April 22, 2021.
Continued insulin injection is a heavy burden on the patient and is a source of concern for the patient’s social life. This latest discovery is the result of basic research in progress, and while the road to clinical application is still far, there are high expectations for steady progress in the future.
(Science Portal Editorial Department Kusaka Takeo)







